
KERATOCONUS INTACTS TREATMENT

Intacs, or corneal inserts, received FDA approval for treating keratoconus in August 2004. These tiny plastic inserts are placed just under the eye's surface in the periphery of the cornea and help re-shape the cornea for clearer vision.
Several studies show that Intacs can improve the best glasses-corrected visual acuity (BSCVA) of a keratoconic eye by an average of two lines on a standard eye chart. The implants also have the advantage of being removable and exchangeable. Intacs might delay but can't prevent a corneal transplant if keratoconus continues to progress.
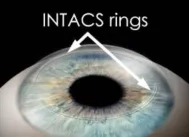
This 15 to 20 minute procedure involves placing plastic inserts just beneath the surface of the eye in the periphery of the cornea. The procedure itself takes approximately 15 to 20 minutes. Topical anesthetic drops are used to numb the eye.
Corneal inserts were typically used when keratoconus patients no longer could obtain functional vision with contact lenses or eyeglasses. However glasses or contact lenses may still be needed after having Intacs inserted. There are other disadvantages of corneal inserts as they can be dislodged at any time with minor trauma. In countries like Canada where Corneal Collagen Crosslinking (CXL) is approved used in combination with excimer laser treatment, Intacs are being used to treat keratoconus less and less since Intacs do not stop the progression of keratoconus. CXL combined with an excimer laser treatment not only stops the progression of keratoconus, but can improve visual acuity as well.
Steps of the Procedure
Step 1: A small incision is made in the corneal surface using either a mechanical tool or a laser.
Step 2: The surgeon places a centering guide on the surface of the eye for several minutes. This helps stabilize the eye and ensure proper alignment of the Intacs. During this time, the corneal layers are gently separated so the Intacs can be inserted.
Step 3: The Intacs inserts are placed. Once completed, the small opening in the cornea is closed with a suture.
As with any surgical procedure, there is a risk of complications. Potential complications include infection, difficulty with night vision, blurred vision and fluctuating vision. It is likely that even after a successful procedure, glasses or contacts are still required.


